Healthcare organizations are starting the transition to a value-based care (VBC) model because it is ultimately better for providers, payers, and patients. But, due to operational challenges, culture, workflows, and resources, moving to a VBC model can be a huge shift for healthcare organizations that’s difficult to get started and manage. Here’s a look at what you need to know about VBC, along with a practical guide to moving from where you’re at today to profitably providing VBC.
Why Transition to Value-Based Care?
Unlike the traditional fee-for-service billing model, value-based care (VBC) requires a healthcare provider to prove to the payer that the care provided is used to improve patient outcomes. Patient care and positive health outcomes are prioritized and incentivized with VBC, making it more worthwhile for healthcare providers to provide the best care for their patients instead of the most care.[1]
Value-based care is about promoting positive health outcomes for patients, above all else. Offering care based on need rather than ordering unnecessary tests that drive up bills is encouraged with the VBC model. Lower costs allow healthcare providers to focus their resources on specialty services that can provide greater positive health outcomes for patients and allow patients to have wider access to care.[1]
The transition to VBC can look different for each organization. Implementing a holistic process and leveraging data can help a healthcare organization develop a VBC payment model that works for patients and is profitable for the healthcare organization. The pressure to reduce healthcare costs and improve outcomes will always be factors healthcare organizations will need to address. Healthcare providers that develop VBC models now may be able to enjoy early advantages that can help them compete in the future. And when the market shifts even further toward providing more value at lower costs, which it inevitably will, those healthcare organizations that have not already started the transition to a VBC model run the risk of being left behind.
The top reasons for healthcare providers to transition to a value-based care model:
- Better patient outcomes
- Reduced total healthcare costs
- Expanded specialty services
- Increased referral revenue
A High-Impact First Step for Transitioning to a Value-Based Care Model: Increase Annual Wellness Visits
Medicare patients and prospective Medicare patients (patients turning 65 in the next 12 months) can be a great first group of patients to target and focus on transitioning to a value-based care model. As part of Medicare, an Initial Preventive Physical Examination (IPPE) visit is paid for by Medicare once per lifetime no later than the first 12 months after a patient’s Medicare Part B benefits eligibility date. This visit is widely known as the “Welcome to Medicare” preventive visit and promotes good health through disease prevention and detection. Medicare covers an Annual Wellness Visit (AWV) that delivers Personalized Prevention Plan Services (PPPS) for patients who aren’t within 12 months of their Medicare Part B benefits eligibility date, didn’t get an IPPE within the past 12 months, and didn’t have an AWV within the past 12 months. The slots allocated for those annual visits often sit unfilled because administrators believe the effort to fill those appointments outweighs the reimbursement value.
Medicare introduced the Annual Wellness Visit (AWV) in 2011 in order to expand coverage of preventive health services to older adults. Providers are able to focus on aspects of preventive care during the AWV (evidence-based screening services, personalized health risk assessments, advance care planning) that may be overlooked during acute problem-based visits because of time constraints or more pressing health concerns. Patients owe no co-pay and healthcare providers are reimbursed at a high rate.[2] “Ideally, the AWV affords the opportunity for early disease detection and downstream mitigation of disease effects, improving patient outcomes and lowering overall costs.”[2]
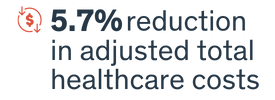
An AWV was associated with significantly reduced spending on hospital acute care and outpatient services. Patients who received an AWV in the index month experienced a 5.7% reduction in adjusted total healthcare costs over the ensuing 11 months.[2]
In addition to the AWV, providers are also able to bill for diagnostic and treatment services provided during the visit, which often results in greater revenue (although these additional services may require a patient co-pay). With only 24% of eligible beneficiaries receiving an AWV in 2017, it is a prime target for growth.[2]
How to Increase Annual Wellness Visits
Before starting a marketing initiative to increase Annual Wellness Visits, it is important to consider:
- The types of information patients receive before they schedule their AWV
- How patients receive information before scheduling their AWV
- How patients can schedule their AWV
- How patients can complete their AWV
- How patients are followed-up with after completing their AWV
Below are some items to consider.
Educate Medicare Patients and Prospective Medicare Patients
Medicare patients, and especially prospective Medicare patients, might not know that an AWV is available to them for free once every 12 months. Also, many Medicare patients are not familiar with the AWV or don’t understand how an AWV is different from an annual physical. It is important to educate Medicare patients on the differences between Annual Wellness Visits and annual physicals, when they are eligible for an AWV, and the costs associated with an AWV (no cost if diagnostic and treatment services are not provided during the visit).
Offer Virtual Annual Wellness Visits in Addition to Office Visits
Given that a physical exam in an office setting is not required for completion of an AWV, a telehealth visit may be an effective, cost-saving way of administering the visit. Older patients might also prefer a telehealth visit versus an office visit due to transportation challenges many of them face, and might be more likely to schedule their AWV if the option is available. Patients can be provided with blood pressure cuffs and scales, as necessary, to facilitate the body mass index calculation and the blood pressure measurement that is required by an AWV.[2]
Utilize Text Messages
A 2021 study found that 61% of U.S. adults ages 65+ own a smartphone.[3] Another study found that appointment reminder response rates were significantly higher for those sent via text message: a 52 percent response rate, compared to 28 percent and 26 percent for email and phone reminders, respectively.
| Appointment Reminder Response Rates | ||
| 52% responses by text message | 28% response by email | 26% responses by phones |
The same study also found that a patient’s preference for text communication is age-agnostic. Text message reminder confirmation rates were 13 percent higher for the 55-74 age group than those aged 18-34. The oldest age group studied (75-94) had a text-based response rate of 39 percent. 56 percent of patients ages 65-84 and 54 percent of those ages 85-94 reply to text reminders to confirm their appointments.[4] It is also important to note that text message appointment reminders are far more effective for seniors if they receive multiple reminders.[5]
| Reply to Text Reminders to Confirm Their Appointments | |
| Ages 65-84: 56% replied | Ages 84-94: 54% replied |
You should also consider the messaging preferences of seniors when creating copy for your text messages. Adults 51+ prefer no emoticon to a smiley face emoticon and “you” statements rather than “we” statements.[5]
If you decide to utilize text messages, make sure the phone number used for sending the text messages is tied to the healthcare organization so that patients know the message is truly from their healthcare provider and not spam. It is also important to review the Telephone Consumer Protection Act (TCPA) to ensure your text messages will be compliant communications.
Best Practices for Annual Wellness Visit Engagement Campaigns
- Leverage Data. Start by focusing a campaign on those patients who are 64 and will be aging into eligibility for an IPPE on their 65th birthday. Once that is underway, design a campaign for those patients who are 65+ and eligible for initial and subsequent AWVs.
- Customize the Message. Most Medicare and Medicare Advantage recipients are either unaware of — or apathetic to — the AWV benefit. Therefore, a campaign should not just be designed around making it easy for an individual to complete their AWV; education should be a core pillar in order to demonstrate the benefit and value of preventive vs. episodic care.
- Measure the Results. Every campaign should deliver real-time data that demonstrates how well the messages are performing. Are they driving click-throughs? AWV appointments? If the results are below expectations, revisit the criteria to ensure the right patients are targeted and that messaging is specific and clear for the call to action. Continue to monitor, measure, and optimize.
- Set Goals. Since AWVs are annual, healthcare organizations see the greatest results when the campaigns run annually. Some organizations launch these campaigns in January when people are thinking about healthy goals and improving behaviors. Others have aligned their launch to Medicare Open Enrollment to ensure patients get the maximum benefits from their coverage. Most importantly, once the AWVs have been launched, they gain the most traction when the campaign is “Always-On”. As the campaigns continue throughout the year, set goals and track progress. With those goals established, find ways to tweak and improve the campaign to meet, and possibly even exceed, your goal. Goals may include:
- Book and complete 95%+ of all AWV appointment capacity annually
- Leverage AWVs to attain HEDIS compliance goals
- Outreach to every patient aging into Medicare this year
- Use AWVs to identify opportunities to expand specialty services
- Identify patients in need of behavioral health or social interventions to improve the health of our senior communities
A Step in the Right Direction
Transitioning from a fee-for service model to a value-based care model can seem like an overwhelming undertaking at first, but in the end it is better for producing positive health outcomes for patients, lowering costs for healthcare providers, providing specialty services and wider access to care for patients, and having more profitable operations for healthcare providers. Focusing on increasing Annual Wellness Visits is a great first step to take for transitioning to a VBC model.
To learn more about how health systems are looking to drive 2x+ in referral revenue and close critical care gaps for patients, read the case study: Annual Wellness Visits Generate Downstream Revenue.

Sources:
[1] What is Value-Based Care?, Babylon Health
[2] Increasing Medicare Annual Wellness Visits in Accountable Care Organizations, The American Journal of Accountable Care, September 15, 2021
[3] Mobile Fact Sheet, Pew Research Center, April 7, 2021
[4] Patients 60% more likely to respond to texts than emails, report finds: 3 notes, Becker’s Hospital Review, January 16, 2020
[5] An exploratory study of mobile messaging preferences by age: Middle-aged and older adults compared to younger adults, SAGE Journals, October 5, 2017

